Confronting the National Opioid Crisis
A Multipart Series
- Introduction
- A Call to Action
- Strategies for Smarter Service
- Expanding Naloxone Awareness and Use
- Doubling Down on Drug Disposal
- Delivering Straight Talk on Opioids
Delivering Straight Talk on Opioids
A mobile clinic in Ohio and public opioid instruction in Florida are prompting conversations and making a difference in those communities.
By Joseph A. Cantlupe
The Ohio Northern University Raabe College of Pharmacy sits on nearly 342 acres in Ada, seemingly the epitome of a quaint small town. The college has been a continual presence in the community, founded in 1884 and graduating thousands of pharmacists over the years. But the community of 6,000 around the campus has been severely struck by the opioid crisis gripping the nation. The area has a mean income of $35,000, with significant poverty and a lack of access to healthcare. Ada has one physician and no specialists.
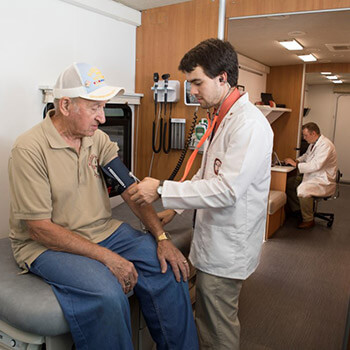
More than three years ago, Dr. Amy Fanous, assistant clinical professor at the college, wanted to show the community what pharmacists can do to help them. She jumped in her Ford Fusion and rambled around, going to churches and schools and neighborhood centers. She took patients’ blood pressure and told residents about preventative health management.
“Amy threw stuff in the back of her car and drove around,” recalled Dr. Steve Martin, dean of the Raabe College of Pharmacy. “She opened an access point.” In 2015, the school received a federal grant, and through donations, it bought a motor coach, dubbed the ONU HealthWise Mobile Clinic. “The original idea was to meet some of the health needs of the community, such as preventative education and management of chronic disease,” Martin recalled.
A switch turned on, too. They began addressing behavioral health and substance abuse issues, including the opioid crisis, which could not be ignored. Student pharmacists became part of the team that roamed the community in the mobile unit, spreading the word about the importance as well as the dangers of drugs and ways people can improve their health. “It opened the door from the opioid perspective,” added Dr. Michael Rush, director of ONU HealthWise.

Around the country, pharmacy schools are enlisting students to become involved as part of their growing effort to demonstrate how pharmacists can help people avoid misuse and abuse of opioids and educate patients about safe and appropriate access to the drugs. Nearly 900 miles away, the University of Florida College of Pharmacy has included students as volunteers to help teach the community about opioid safety issues. Student pharmacists talk with residents about the signs of opioid misuse and discuss proper drug storage, the best way to dispose of medications and how naloxone can reverse opioid overdoses.
Student pharmacists now comprise at least a third of the program’s community trainers, who have served 1,000 people since August 2017, said Dr. Carol Anne Motycka, the assistant dean, campus director and clinical associate professor who originated the program. Bringing student pharmacists into the community has long been part of Motycka’s instruction, whether it’s going to the crime laboratories or drug courts “and letting them see what people are dealing with.”
The opioid issue brought home the need to step up instruction surrounding substance abuse and pharmacists’ role in the community, said Motycka. “We’ve always tried to do some training, but honestly it hasn’t been the big issue that it is now. The last several years we really ramped it up.” Motycka is also co-chair of the Heroin and Opioid Task Force, which is part of a Duval County community organization named Drug Free Duval where she works with community partners to deal with substance abuse issues.
The training is now considered part of the curriculum, and students volunteer and then help train people in the community “not only about all the signs of misuse and the red flags about opioids, but how you can help people” with screenings, interventions and referrals for treatment, she said.
It’s one thing to talk academically about the drug usage problems; it’s another to see it firsthand. “I think all of us live in a little world of our own,” she added. “We don’t get to see some of the stuff that’s going on. You might hear about it with the media but you need to actually talk to the folks dealing with this stuff. As pharmacists, we are one of the more accessible providers in healthcare.”
A Wake-Up Call in Ohio
In Ada, the local media described the community as a breeding ground for opioid use. The numbers from the courthouse told the story: Five years ago, the courts counted zero opioid-related cases. Now, non-prescription opioids account for 21 percent of cases, the media reported.

“We’re in a community where opioid use, heroin use is a big deal,” Martin said. ”You wouldn’t think of it in a sleepy town like Ada, but it is, it definitely is. We’ve been watching this whole thing unfold over the course of several years. And we have a tool that might be able to address some of the needs in the area. We have a community that needs this assistance, and part of our mission is community engagement. From the get-go, the whole idea was to bring access to the healthcare system for our community.”
Students are an integral part of the teams in the mobile clinic, under the supervision of a licensed professional. At least two pharmacy students occupy the mobile unit at a time. They go out from one to five days a week, said Fanous, now director of the ONU HealthWise Mobile Clinic. Sometimes they go to a parking lot, stay there and meet local residents. Sometimes they go to food pantries and win over local residents by helping them clean dishes or carry food. “It’s become a key component of the education we are providing the students,” Rush noted.
Making inroads into helping patients in their everyday care is part of the mobile clinic’s role, including addressing some issues that are not often discussed, such as proper medication disposal. In Hardin County, where Ada sits, not many medication disposal sites exist and some people might be reluctant to use the program run by the sheriff’s department, Rush said. To alleviate that problem, the mobile clinic provides patients with bags to discard their old medications to deactivate the drugs. “We don’t have to worry about the drugs getting into the wrong hands. It’s a critical piece of the puzzle,” Rush said.
For many people, opioid use is linked to their struggles with overcoming and managing pain. With the mobile clinic, students “have the opportunity to talk to patients about how to manage pain, how to use medicine to control pain and other non-medication strategies to control pain,” Martin pointed out. “That’s an important piece for us. It’s important we’re talking about their use of prescription drugs. No one wants to be addicted to pain medication, but we make people aware that’s a possibility and help them manage through controlling pain in an appropriate way. Those are solutions that we as pharmacists can provide anywhere.”

The mobile clinic’s many roads through the community are “eye-openers” for the students. Becoming involved and watching the discussions has a profound impact. They see the quizzical looks from the residents and the uncertainty about their health. Fanous talked about how one resident had high blood glucose but it didn’t affect him until he mentioned he had trouble seeing. That raised alarms within the mobile unit and the team worked to get him follow-up care for diabetes. “For some individuals, this is the only access he or she may have to healthcare,” said student pharmacist Megan Stephan.
The mobile clinic is putting on the miles, partnering with the local health center, the health department and the critical access hospital in the area, Hardin Memorial Hospital. The clinic has averaged 400 healthcare events annually. At least 27 percent of patients return for follow-up visits. According to the college, at least 47 percent of patients had abnormal clinical findings and about 17 percent of patients were referred to a physician for care management, including acute care concerns.
Student pharmacist Clayton Miller said he has witnessed amazing moments. “Simply even talking to a patient that comes into the mobile clinic or even letting them know their blood pressure is a little bit high might be the one step that prevents them from having a serious medical-related event that could be fatal.”
Sparking Conversations in the Sunshine State
The Jacksonville, Florida, area has been particularly hard hit by opioid problems. In 2017, the Jacksonville Fire and Rescue Department handled 3,460 overdose calls, an average of 308 per month, according to department records. At least 10 percent of overdose calls in 2017 were repeat occurrences. And 2 percent of those patients with repeat occurrences had them 10 or more times.
With the city and nearby communities battling opioid issues, the University of Florida pharmacy program revamped its training modules in the curriculum related to opioid instruction. Students who volunteer discussing opioids in the community may receive instruction and can become trainers themselves, accompanied by academic supervisors. During the training, they teach the community how to screen and provide interventions in locations such as homeless shelters or at facilities for foster parents and then provide referrals for treatment if needed. At least one-third of the trainers—about 50 so far—have been students.

The student pharmacists also quiz people involved in helping patients deal with opioids and talk with high school and middle school students about the drugs. They discuss the dangers of “pharm parties,” where people give drugs to partygoers, who may not know what they are taking. To demonstrate, they hand out bags of different colored Skittles representing various pills. Ensuing confusion shows the students how easily trouble comes.
“So you took the blue one and the red one, now what’s going to happen because of the interaction?” Motycka said, recounting the exchanges. The student pharmacists “talk to the high school students and it hits home with them. They do a better job than I do when they go to schools. The students really listen to them because they are closer in age,” Motycka said. “You can talk until you are blue in the face but without showing them, it doesn’t make much of an impact.”
Residents in the community ask questions about drug use and the trainers then check afterward to ask how much they learned. Many people lack understanding about the intricacies of opioids. For instance, many don’t realize that heroin is an opioid and it can be taken orally or smoked, Motycka said. The student pharmacists review the many elements of opioids with the residents. “It’s incredible in general how little knowledge is out there before [they are] trained,” she noted.
The sessions are a big draw for the students. “Honestly, they do it on their own time but they love it and even say it’s an amazing experience, they’ll do it again.” Student pharmacist Ekaterina Nichols volunteered to discuss pharmacological issues at the local homeless shelter and the experience humbled her. When they distributed and discussed the material, Nichols was at first worried about how people would accept the material. “To my surprise the public was very receptive and forthcoming,” Nichols said. Not only that, many people asked for more information or where they could get assistance if a loved one or relative fell victim to opioid abuse. They also sought more information about ways to combat opioid abuse.
“This teaching experience was of paramount importance to me as a future pharmacist because it underlined the public need for education on opioid-related issues,” Nichols said. ”I felt that my teaching was extremely helpful to the public. Most important, it gave me the opportunity to interact with a vulnerable population whose needs are often overlooked. The experience was humbling and I would gladly repeat it again.”
As Motycka examines her program, she is hopeful that their efforts are making an impact in the area. “Hopefully once [the students] are pharmacists, they are going to continue doing this,” she said. “One of the things we emphasize is that we can make a huge difference in the community.”
Joseph A. Cantlupe is a freelance writer based in Washington, D.C.

