Pharmacy Education 2026 Call for Roundtable Topics
In November 2023, the AACP Strategic Planning Committee (SPC) launched strategic planning efforts to develop a plan to guide the Association for the next cycle, years 2024-2026. Using the “continuous strategy process”, our strategic efforts and plans do not have a set “stop date”. This allows us, over a shorter time period and on an ongoing basis, to be more nimble, more responsive, and more proactive regarding the issues and concerns facing the pharmacy academy and profession.
Interim Meeting 2026: Post-Meeting Survey

Conversations That Matter: The AACP Interim Meeting 2026
Sheraton Puerto Rico
February 14-17, 2026
Thank you for attending Conversations That Matter: The AACP Interim Meeting 2026. Please take a few minutes to complete this brief survey and share your feedback about the meeting. We value your input, and your comments will assist us in planning future events.
This survey will close on Tuesday, March 6. Your responses to this survey will remain confidential.
Payment for Faculty-Provided Patient Care Services

AACP Workgroup on Payment for Faculty-Provided Patient Care Services
Advancing payment through education, advocacy, and partnerships
Background
The AACP Pharmacy Faculty Clinical Service Reimbursement Workgroup was originally formed as a Council of Deans Task Force in July 2024. Its initial charges focused on a comprehensive review of clinical faculty payment models, including an analysis of the 2022 patient care survey data that originated from the 2021-22 AACP Strategic Engagement Committee, and the creation of a new survey for pharmacy deans. The task force engaged with key experts in billing and compensation and successfully launched an updated survey to member institutions in late 2024. Building on these accomplishments, which included finalizing survey analysis and developing manuscripts for publication and presentation, the group recommended its elevation to an ongoing workgroup for the Academy. This decision was based on the recognition that the complexities and evolving nature of pharmacy practice faculty payment require a continuous, dedicated effort to advance advocacy, education, and resource development within the Academy. Efforts of this group will also align with and be supported by the AACP Transformation Center and the ACT Pharmacy Collaborative.
Workgroup Members
- Ashley Ellis, The University of Tennessee Health Science Center
- Don A. Godwin, University of New Mexico
- Paul Gubbins, University of Missouri-Kansas City (Vice Chair)
- John Gums, University of Florida (Chair)
- Randy McDonough, Loma Linda University
- Magaly Rodriguez de Bittner, University of Maryland
- Todd Sorensen, University of Minnesota
- Kristen Wiisanen, Rosalind Franklin University
Evergreen Charges
- Payer Engagement & Strategy: Cultivate strategic relationships with payers (e.g., commercial insurers, Medicaid, commercial Medicare Advantage partners) and relevant stakeholders, including health system executives and healthcare improvement companies (e.g., Vizient), to understand their priorities and the value of pharmacist-provided patient care services. This may include developing resources, engaging in listening sessions, and conducting pilot studies to identify and promote innovative payment models for pharmacist-provided care.
- Advocacy & Education: Serve as the primary advocate for the payment of patient care provided by pharmacy faculty by developing and disseminating consistent, yet flexible, educational resources and talking points for deans, chairs, faculty, staff, and students. This also includes strengthening relationships with state-level partners and national organizations to advance supportive legislation and policy.
- Resource Development & Knowledge Exchange: Establish and maintain a dynamic resource hub that provides guidance on pharmacist-provided patient care faculty payment and reimbursement models. This may include creating a living repository of successful practices, FAQs, and a consultant or coaching model to facilitate knowledge exchange and support individual colleges and schools in developing their own strategies.
2025-2027 Workgroup Goals
Payer Engagement & Strategy:
- Conduct "Listening Sessions": Organize and host at least three virtual listening sessions or focus groups with key representatives from diverse payer types (e.g., Medicare Advantage, commercial, self-insured). The goal is to identify their top priorities and barriers to reimbursing pharmacist services.
- Launch a Pilot Program: Partner with one member institution to design and implement a pilot study to test a novel payment or care coordination model identified in the listening sessions, with a clear plan for data collection and outcome measurement.
Advocacy & Partnerships
- Create Consistent Messaging: Develop and publish a core set of advocacy talking points and other resources that can be utilized by academic pharmacy leaders to discuss the value of patient care services provided by pharmacy faculty with policymakers and other stakeholders.
- Develop Payer-Focused Resources: Create a suite of resources (e.g., a "Payer Toolkit" or a series of case studies) that distills the findings from the payer listening sessions and provides evidence-based talking points for academic pharmacy leaders when engaging with payers, legislators, and other stakeholders.
- Partner with National Stakeholders: Collaborate with at least one national partner organization (e.g., ASHP, APhA, NCPA or NASPA) to disseminate the Workgroup's findings and/or on a collaborative project.
Resource Development & Knowledge Exchange
- Launch a Digital Resource Hub: Create a dedicated section on the AACP website that serves as a living repository of the Workgroup's findings, best practice examples of faculty contracting, and a comprehensive FAQ based on common questions from the Academy.
- Enhance AACP's Mentorship Program: Integrate specific content on pharmacist-provided patient care service compensation strategies for faculty into the existing AACP CEO Dean Mentorship Program, and explore the consultancy model for broader implementation.
- Facilitate Peer-to-Peer Exchange: Establish a formal, volunteer-driven "coaching" or "consultant" resource for member institutions to provide one-on-one guidance on developing and expanding pharmacist-provided patient care service compensation strategies using published findings and impact form the workgroup.
Publications & Resources
K. Wiisanen, P.O. Gubbins, J.G. Gums, et al., "Recognizing the Value of the Practice Enterprise: Billing for Faculty Patient Care Services to Strengthen Education and Advance the Profession," American Journal of Pharmaceutical Education 90, no. 2 (2025), 10.1016/j.ajpe.2025.101924.
J.G. Gums, C.P. Henchey, T.C. Dowling, et al., "National Assessment of Reimbursement Models for Clinical Faculty Services in Academic Pharmacy Practice," Journal of the American College of Clinical Pharmacy 8, no. 12 (2025): 1226-1232, https://doi.org/10.1002/jac5.70134.
2025 Council of Deans (COD) Payment of Clinical Faculty Services Taskforce Final Report
Pharmacist Professional Patient Care Practice Resources
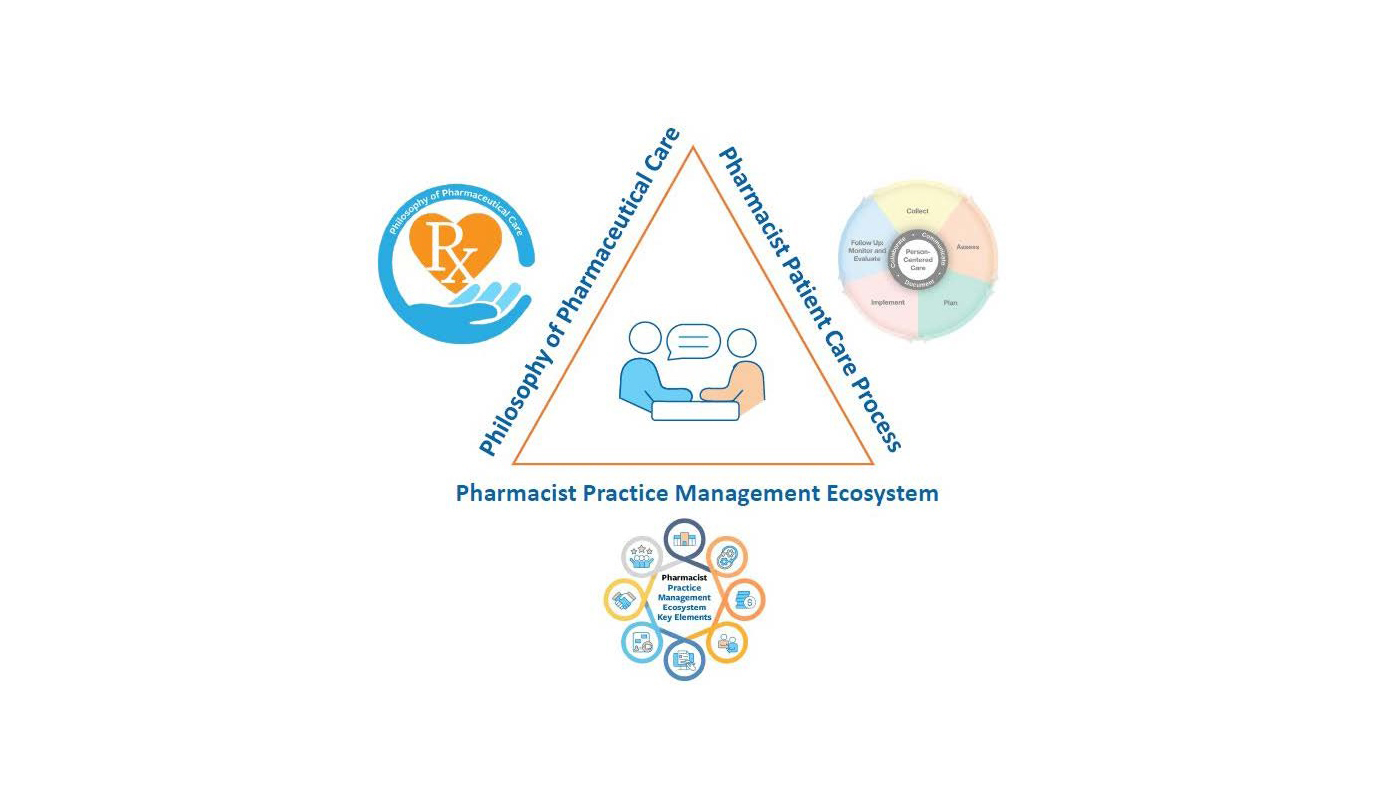
Components of a Pharmacist Professional Patient Care Practice
Today's pharmacists are medication experts whose services are growing as a result of practice expansion through state laws and regulations, health practitioner collaborations, and sustainable payment for patient care services. Comprehensively defining the key elements of a pharmacist professional patient care practice is vital to foster replicable, standardized, and sustainable pharmacy practices serving the needs of patients nationwide to achieve broader healthcare goals including improved health outcomes and cost-effective care.
Throughout health care, there are three core components of a professional patient care practice: Philosophy of Practice, Patient Care Process, and Practice Management System. These core components are universally accepted across each health profession. The profession of pharmacy has defined and broadly adopted each of these core components: the Philosophy of Pharmaceutical Care (1990), the Pharmacists' Patient Care Process (2014 and updated 2025), and the Key Elements of a Pharmacist Practice Management Ecosystem (2026).
Philosophy of Pharmaceutical Care
Pharmaceutical Care is a person-centered practice in which the practitioner assumes responsibility for a patient's medication-related needs and is held accountable for this commitment.1 The pharmacy profession recognized the need for unified language of how to directly apply the philosophy of pharmaceutical care to individual patients first through the Core Elements of Medication Therapy Management 1.02 and 2.03, then in 2014 and 2025 through the JCPP Pharmacists’ Patient Care Process4,5, now adopted across all colleges and schools of pharmacy through the 2016 and 2025 ACPE Accreditation Standards6,7.
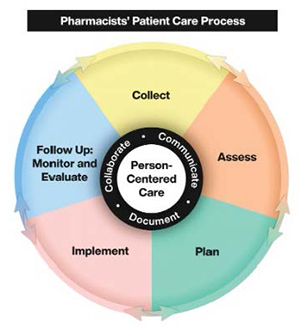
Pharmacists' Patient Care Process
The Pharmacists' Patient Care Process (PPCP) is a consistent and standardized five step process (COLLECT, ASSESS, PLAN, IMPLEMENT, FOLLOW-UP) guided by evidence, clinical reasoning, and complexity of patient needs where pharmacists support patients to meet their medication and health outcomes.5 The PPCP is applicable across all practice settings and modes of delivery (e.g., in person, telehealth), and is optimized when pharmacists have access to contemporary technology capabilities that augment their practice, enable documentation of their services, and allow for secure exchange of patient information through standardized data-sharing solutions.5
More information on the Pharmacists' Patient Care Process can be found on the Joint Commission of Pharmacy Practitioners website.
Pharmacist Practice Management Ecosystem
The Pharmacist Practice Management Ecosystem is a dynamic system, grounded in eight interdependent key elements that are needed to establish, maintain, and grow a pharmacist patient care practice in any setting.6 The ecosystem in which the practice operates goes beyond the pharmacy practice itself and is informed by pharmacists, their professional teams, organizational structures, and the surrounding healthcare environment. Pharmacists and their teams engage within the ecosystem to deliver expert medication-related health care while adapting to regulatory, economic, and technological advances, ensuring sustainable patient care services.
More information on the Pharmacist Practice Management Ecosystem can be found on the Joint Commission of Pharmacy Practitioners website.
Citations
- In: Cipolle RJ, Strand LM, Morley PC. eds. Pharmaceutical Care Practice: The Patient-Centered Approach to Medication Management Services, 3e. The McGraw-Hill Companies; 2012.
- American Pharmacists Association, National Association of Chain Drug Stores Foundation. Medication therapy management in community pharmacy practice: core elements of an MTM service (version 1.0). J Am Pharm Assoc2005;45:573-9.
- American Pharmacists Association; National Association of Chain Drug Stores Foundation. Medication therapy management in pharmacy practice: core elements of an MTM service model (version 2.0). J Am Pharm Assoc 2008; 48(3):341-53. doi: 10.1331/JAPhA.2008.08514. PMID: 18595820
- Joint Commission of Pharmacy Practitioners. Pharmacists’ Patient Care Process-May 29, 2014. https://jcpp.net/wp-content/uploads/2016/03/PatientCareProcess-with-supporting-organizations.pdf. Accessed February 6, 2026.
- Joint Commission of Pharmacy Practitioners. Pharmacists’ Patient Care Process-May 20, 2025. https://jcpp.net/wp-content/uploads/2018/10/Pharmacists-Patient-Care-Process-Document-2025.pdf Accessed February 6, 2026.
- Joint Commission of Pharmacy Practitioners. Key Elements of a Pharmacist Professional Patient Care Practice: Pharmacist Practice Management Ecosystem. February 6, 2026. Available at: https://jcpp.net/patient-care-process/jcpp-key-elements-of-a-pharmacist-practice-management-ecosystem.
AACP NMA Workshop - Sponsorship Opportunities
The primary objective of the one-day Self-Care Workshop, which immediately precedes AACP PharmEd 2026 (AACP’s annual meeting), is to bridge pharmacy education and practice by covering educational topics in self-care and community practice to advance the pharmacist’s role.
More than 125 educators with interest in self-care therapeutics, outpatient pharmacy practice, and/or public health will come together to:
ACT Task Force
The ACT Pharmacy Collaborative Task Force provides strategic leadership and guidance to advance community-based pharmacy practice transformation. The Task Force brings together pharmacy educators, national pharmacy organizations, practice partners, and AACP staff to set priorities, guide initiatives, and foster collaboration across education and practice.
Letters & Statements - Archives

Letters & Statements: 2026 | 2025
Statements
AACP Supports Statement from AAI and ACP Emphasizing the Critical Role of Vaccinations in Public Health (March 18, 2025)
FASHP Statement on NIH Funding Reductions (February 15, 2025)
Letters
CHF Letter to Appropriators on Leaked HHS FY26 Discretionary Budget Passback (April 25, 2025)
Friends of NCHS Recommendation for FY26 (April 24, 2025)
FY 2026 ARPA-H Community Letter (April 23, 2025)
AACP Supports the Friends of VA Medical Care and Health Research FY26 Recommendation for the Medical and Prosthetic Research Program (April 14, 2025)
AACP Supports the CDC Coalition in FY26 Recommendations for CDC (April 9, 2025)
AACP Joins 500+ Organizations in NIH FY26 Funding Recommendation (April 8, 2025)
AACP Joins 50+ Organizations in NIAID FY26 Funding Recommendation (April 7, 2025)
AACP Joins American Council on Education (ACE) Comment Letter on White House AI Action Plan (March 14, 2025)
FASHP’s Letter on Reconciliation and Student Loans Borrowers (March 7, 2025)
AACP Supports Updates to DEA Registration for Pharmacists (March 3, 2025)
AACP Joins Friends of AHRQ Letter on FY26 Appropriations (March 3, 2025)
AACP Signs on to FY25 NIH Funding Community Letter (February 25, 2025)
The American Society of Health-System Pharmacists (ASHP), American Pharmacists Association (APhA), American Association of Colleges of Pharmacy (AACP), and American Association of Psychiatric Pharmacists (AAPP) released a joint statement on the violence in Minnesota: